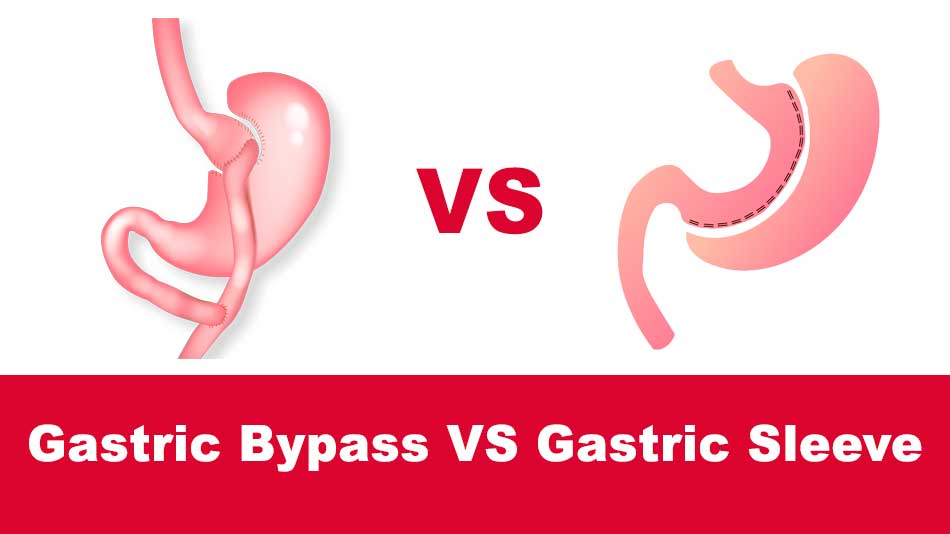
Gastric sleeve vs gastric bypass: what’s the difference?
When it comes to bariatric surgery, two of the most common options are gastric sleeve and gastric bypass. Both procedures help people lose weight by altering the digestive system, but the way they do so varies significantly. Understanding the difference between these two procedures can be critical in making an informed decision based on your health and weight loss goals.
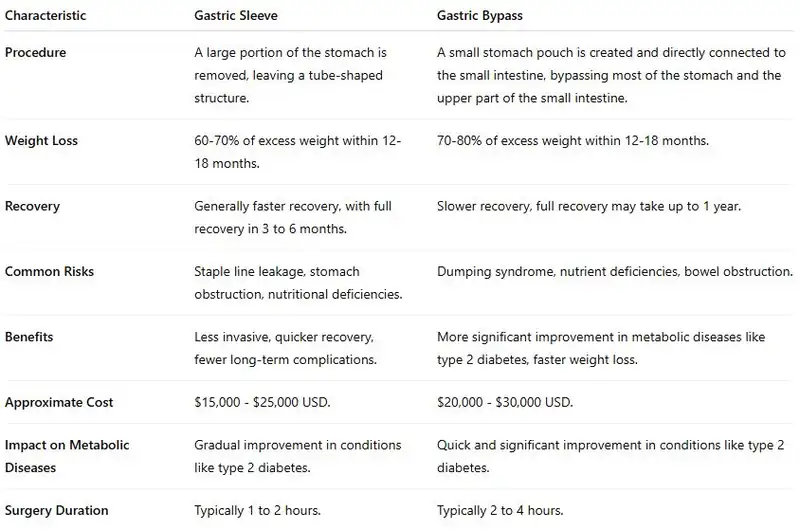
Comparison Chart
Comparison table of both bariatric surgeries
Overview of gastric sleeve
Gastric sleeve surgery, or sleeve gastrectomy, is a procedure that involves removing a significant portion of the stomach. The remaining stomach takes the shape of a tube or sleeve, much smaller than a normal stomach. This drastic reduction in stomach capacity makes patients physically unable to consume large meals, and the procedure often leads to significant weight loss.
One of the main advantages of gastric sleeve surgery is that it also affects hormone levels in the stomach, particularly the hormone ghrelin, which is responsible for feelings of hunger. By removing a large part of the stomach, the production of this hormone is reduced, which helps patients feel less hungry during the day. This can make it easier to follow a low-calorie diet, as patients do not feel the need to eat as often or in large quantities.
In addition, gastric sleeve has the advantage of being a less complex procedure than gastric bypass. It does not involve rerouting the intestine, which often makes it a simpler procedure with fewer risks during the operation. The recovery time for gastric sleeve is usually shorter than for gastric bypass, making it a popular choice for those seeking a less invasive approach.
How gastric bypass works
Gastric bypass, or Roux-en-Y gastric bypass (RYGB), is a more complex procedure than gastric sleeve. It involves creating a small pouch at the top of the stomach, which is then connected directly to the small intestine, bypassing most of the stomach and the upper part of the small intestine. This alters both the stomach’s ability to hold food and the way the body absorbs nutrients.
The bypass causes both a restriction in food intake and a reduction in calorie absorption. Food bypasses most of the stomach and the duodenum, the first section of the small intestine, resulting in less absorption of essential nutrients. This is one of the reasons why patients who undergo gastric bypass surgery tend to experience greater weight loss than patients who undergo gastric sleeve surgery in the early stages, as reduced nutrient absorption contributes directly to faster weight loss.
However, bypass surgery has a significant disadvantage: it requires a complete restructuring of the digestive system, which increases the risk of complications such as vitamin deficiencies and digestive problems. This surgery also usually involves more drastic lifestyle changes, as patients must strictly follow dietary recommendations and take supplements to prevent long-term nutritional deficiencies.
Advantages of gastric sleeve and gastric bypass
Both procedures have been shown to help people lose weight and improve their health, but they offer different advantages depending on the patient’s medical needs, health status, and weight loss goals.
Weight loss expectations
In patients who undergo gastric sleeve surgery, weight loss is usually significant, with most people losing between 60% and 70% of their excess weight in the first 12 to 18 months. However, weight loss may be more gradual than with gastric bypass surgery. Gastric sleeve surgery is often recommended for patients with moderate to severe obesity and is especially effective for those who are committed to making the necessary lifestyle changes to maintain their weight loss.
On the other hand, gastric bypass surgery tends to result in faster weight loss, with many patients losing 70% to 80% of their excess weight in the same time frame. This is partly because the procedure limits both the amount of food that can be eaten and the amount of nutrients that are absorbed. Gastric bypass is often recommended for people with more severe obesity or who have obesity-related conditions such as type 2 diabetes, as it can offer faster improvements in these areas.
However, faster weight loss can lead to a number of problems. Patients who lose weight too quickly may experience muscle loss, nutritional deficiencies, or other complications that must be monitored closely.
Long-term health improvements
One of the most notable benefits of both gastric sleeve and gastric bypass is their ability to significantly improve or even resolve obesity-related health conditions. These include type 2 diabetes, hypertension, sleep apnea, and high cholesterol. In fact, studies show that more than 80% of patients with type 2 diabetes experience remission or improvement after undergoing gastric sleeve or gastric bypass surgery.
Gastric bypass, in particular, has been shown to have more dramatic effects on metabolic diseases such as diabetes. The rerouting of the small intestine helps improve insulin sensitivity, which can lead to better blood glucose control in patients with diabetes. Many patients find that they can stop taking diabetes medications within a few months after surgery, thanks to their body’s improved ability to process sugar and insulin.
Although gastric sleeve surgery also helps with weight-related diseases, it tends to have a slower impact on conditions such as diabetes. However, for patients with milder forms of these diseases or no other significant health problems, gastric sleeve surgery may still be a very effective option for improving long-term health.
Risks and complications of each procedure
As with any surgery, both gastric sleeve and gastric bypass carry risks that must be considered. Understanding these risks is essential to making an informed decision about which surgery is best suited to an individual’s needs.
Common risks of gastric sleeve
Leaks: After gastric sleeve surgery, there is a minimal but real risk of leaks occurring at the suture line where the stomach has been stitched. Although this is a rare occurrence, it can lead to infection and, in some cases, additional surgery may be required to repair the leak.
Stomach obstruction: Since the stomach is much smaller after surgery, there is a risk that food may become stuck, causing nausea or pain. This condition, known as “stomach obstruction,” can sometimes be treated with minor medical intervention, but in more severe cases may require additional surgery.
Nutritional deficiencies: With the reduction in stomach size, patients are at risk of developing deficiencies in essential nutrients, particularly vitamin B12, iron, and calcium. For this reason, rigorous intake of vitamin supplements is essential for patients undergoing gastric sleeve surgery in the long term.
Risks associated with gastric bypass
Dumping syndrome: One of the most common complications for patients undergoing gastric bypass is dumping syndrome. This condition occurs when food passes too quickly from the stomach to the small intestine, causing symptoms such as nausea, diarrhea, dizziness, and fatigue. It is usually caused by eating sugary or high-fat foods.
Nutritional deficiencies: Since gastric bypass diverts the path of the intestine, it reduces the absorption of vital nutrients. Patients are particularly prone to deficiencies in vitamin D, vitamin B12, iron, calcium, and protein. Regular supplements and blood tests are needed to monitor these levels and prevent serious complications.
Intestinal obstruction: Another potential risk of gastric bypass is intestinal obstruction, which occurs when the intestine becomes blocked. This can cause severe pain, nausea, and vomiting, and may require medical attention.
Recovery process: What to expect after surgery
Recovery is an essential part of both gastric sleeve and gastric bypass surgery, and the post-operative experience can vary between the two procedures. Although both procedures involve lifestyle changes and a period of physical recovery, patients who undergo gastric bypass surgery typically have longer recovery times due to the complexity of the procedure.
Recovery time after gastric sleeve
Recovery after gastric sleeve is usually faster than after gastric bypass, with most patients only staying in the hospital for one or two days. Patients can begin eating solid foods within four to six weeks, following a carefully monitored eating plan that includes a transition from liquids to pureed foods and eventually to solid foods.
During the first few weeks, patients may experience fatigue and discomfort as their bodies adjust to the reduced food intake. It is also important for patients to avoid strenuous activities, including weight lifting, for approximately six weeks after surgery. After this period, many patients can resume their normal daily activities and begin to incorporate light physical exercise into their routine.
Recovery after gastric bypass
Gastric bypass surgery requires a longer recovery time due to the complexity of the procedure. Most patients stay in the hospital for about two to three days after surgery and gradually reintroduce solid foods over several months. During the initial recovery period, patients will follow a liquid diet, which will gradually transition to blended foods and then solid foods.
It can take up to 12 weeks before patients feel fully recovered and return to their normal activities, although for some people, full recovery may take a year or more. The more invasive nature of gastric bypass requires careful follow-up monitoring and dietary adjustments to ensure that the patient’s body adapts to the changes without complications.
Cost comparison: gastric sleeve vs. gastric bypass
When considering weight loss surgery, cost is an important factor for many patients. Both gastric sleeve and gastric bypass come at a significant cost, but there are differences that may influence a patient’s choice.
Average costs and insurance coverage
The cost of gastric sleeve surgery typically ranges from $15,000 to $25,000 in the United States, depending on the location, surgeon, and specific healthcare provider. Insurance coverage may vary, but many health plans cover the surgery if certain criteria are met, such as a body mass index (BMI) greater than 40 or a BMI greater than 35 with obesity-related medical conditions.
Gastric bypass tends to be slightly more expensive, with costs ranging from $20,000 to $30,000. Like gastric sleeve, it may be covered by insurance, although the patient must meet specific medical criteria to be eligible for coverage. Both surgical procedures usually involve additional costs for consultations, follow-up visits, and post-operative care.
Hidden costs to consider
Both procedures involve hidden costs in addition to the initial procedure. For patients undergoing gastric sleeve surgery, the need to take vitamin and mineral supplements for life can add additional costs over time. Similarly, patients who undergo gastric bypass surgery face higher long-term costs due to the need for more frequent medical follow-up, additional dietary supplements, and possible treatments for complications such as nutritional deficiencies.
How to choose between gastric sleeve and gastric bypass
Choosing the most appropriate weight loss surgery is a personal decision that depends on several factors. It is important to carefully evaluate your weight loss goals, medical history, and preferences before making a decision.
Factors to consider before choosing
Severity of obesity: Gastric bypass is often recommended for people who are more severely obese or who need to lose a large amount of weight quickly. It may also be recommended for people who have obesity-related conditions, such as diabetes.
Risk tolerance: Gastric bypass carries a higher risk of complications than gastric sleeve, so patients should consider their tolerance for such risks before making a decision.
Personal preferences: Some patients may prefer gastric sleeve because it is less invasive, has a shorter recovery time, and carries fewer long-term complications. Others may opt for gastric bypass because of its greater impact on rapid weight loss and metabolic improvements.
Medical consultation and advice
Ultimately, the decision should be made in consultation with a doctor who specializes in bariatric surgery. A surgeon can offer personalized advice based on the patient’s medical history, health goals, and weight loss expectations.
Who qualifies for bariatric surgery?
Bariatric surgeries, either gastric sleeve or gastric bypass, are not for everyone. These procedures are recommended for patients who have a specific body mass index (BMI) and who have tried unsuccessfully to lose weight through traditional methods.
Long-term considerations after surgery
Both gastric sleeve and gastric bypass require a long-term commitment to maintain weight loss and overall health. These surgeries are not quick fixes, but tools that help people make lasting lifestyle changes.
Lifestyle changes after surgery
After surgery, patients who undergo gastric sleeve or gastric bypass surgery must make significant lifestyle changes. These include following a strict diet, engaging in regular physical activity, and taking supplements for the rest of their lives. Failure to follow these guidelines can lead to weight regain and other complications.
Maintaining weight loss over time
Maintaining long-term weight loss after surgery requires consistent effort. Regular physical activity, mindful eating habits, and emotional support are essential for maintaining weight loss. Regular check-ups with medical professionals ensure that any issues, such as nutritional deficiencies or weight gain, are detected early.
Our doctors are ready to help you choose the best bariatric surgery to achieve your weight loss goals.

About the Author: Dr. Mario Camelo
Specialty: Bariatric Surgery and Advanced Laparoscopy
Dr. Mario Camelo is a leading bariatric surgeon in Tijuana, Mexico, with over 15 years of experience in weight loss surgery. Specialized in minimally invasive techniques, he has successfully performed procedures such as gastric sleeve, gastric bypass, revision surgeries, and Single-Incision Laparoscopic Surgery (SILS).
He specialized in advanced laparoscopy through a fellowship at Hospital Ángeles Tijuana and complements his practice with ongoing medical education. He is currently part of the Bariatrics MX team, and is certified by the Mexican Board of General Surgery.